Doulas are making a difference for families worldwide.
DONA International is the leader in evidence-based doula training, certification and continuing education. Our doulas are the world's best! What is a doula?
I want to FIND a doula.
Parents, DONA International can help you connect with a professional, highly skilled birth or postpartum doula in your area.

I want to BECOME a doula.
It’s an incredible time to start your journey as a birth or postpartum doula. Let’s explore this path together.
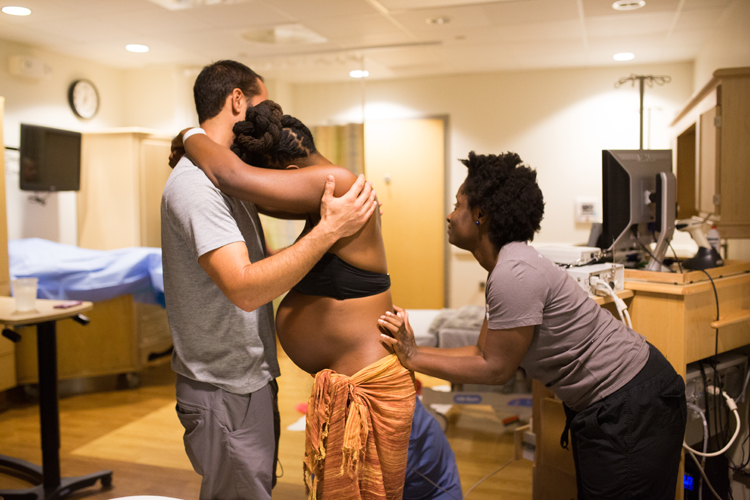
I AM a doula.
We’d love to have you join thousands of doulas around the world as a member of DONA International.
“If a doula were a drug, it would be unethical not to use it.”
Continuing Education
DONA International offers in-person and online webinars for continuing education for our doulas and birth professionals alike!
This year the DONA Summit will be held 100% online. Rotating between in-person and virtual conferences allows for more access to birth and postpartum professionals from around the world! The virtual conference will be live on October 28-29, 2024; with all sessions available on-demand for 60 days after the live days as well. Visit our annual conference website and continuing education page to find a learning experience to enhance your doula skills (practice) or doula business.
More Conference Information >>
Continuing Education Information

We’re Here for You
DONA International is member driven and we are here to support you! Connect with the professional staff in our home office, a member of the board of directors or your state/regional representative.
Reporters and Editors… Let’s talk!
Every week, DONA International is contacted by reporters and editors around the world. As representatives of the world’s leading doula organization, we’d love to talk as we increase awareness about the benefits of doula support to families globally!
DONA International and our doulas have contributed to many articles including pieces by The New York Times, Essence magazine, The Washington Post, The Bump, Fit Pregnancy, and more!


Acompañar en la Incomodidad
Muchas veces nos toca acompañar ahí, en ese océano en el cuál se sumerge la mujer recién parida. En ese puerperio abrumador, donde su identidad queda confundida y aplastada por el derrumbe que originó el ingreso a la maternidad. Y entonces se nos plantea otra vez el...

How to Get your First Doula Clients
Once you complete your DONA International doula training you’ll have all of the knowledge and skills you need to get out there and start serving pregnant people and new families. Then It’s time to find those first three certifying families to support! It can be...

Becoming a Doula: Tips for a Career Switch
This past year has been a tumultuous one for most people. The emergence of COVID-19 turned our world upside down as our loved ones fell ill, our children schooled from home and our employment changed in major ways. It was, and still is, a time of drastic adjustment,...
The Rise of the Virtual Doula
In early 2020, when COVID-19 began to spread across the world, and most hospitals and birth centers revised their visitor policies, many doulas scrambled to offer their clients the best support they could over the phone via FaceTime, or through a webcam set up in...

